These are the first symptoms of cr…See more
These are the first symptoms of cr…See more
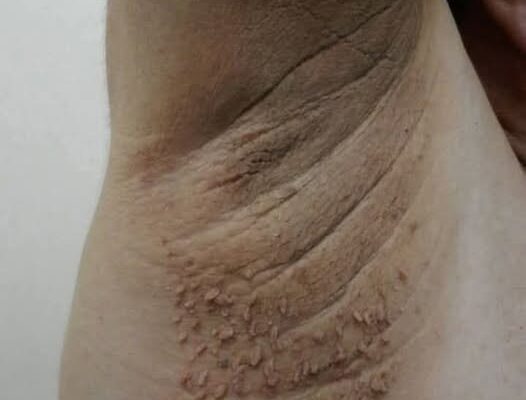
Have you or someone you know noticed dark, velvety patches of skin on the back of the neck or under the arms? While it may look like a buildup of dirt, this skin change could be a sign of an underlying health issue — one that shouldn’t be ignored.
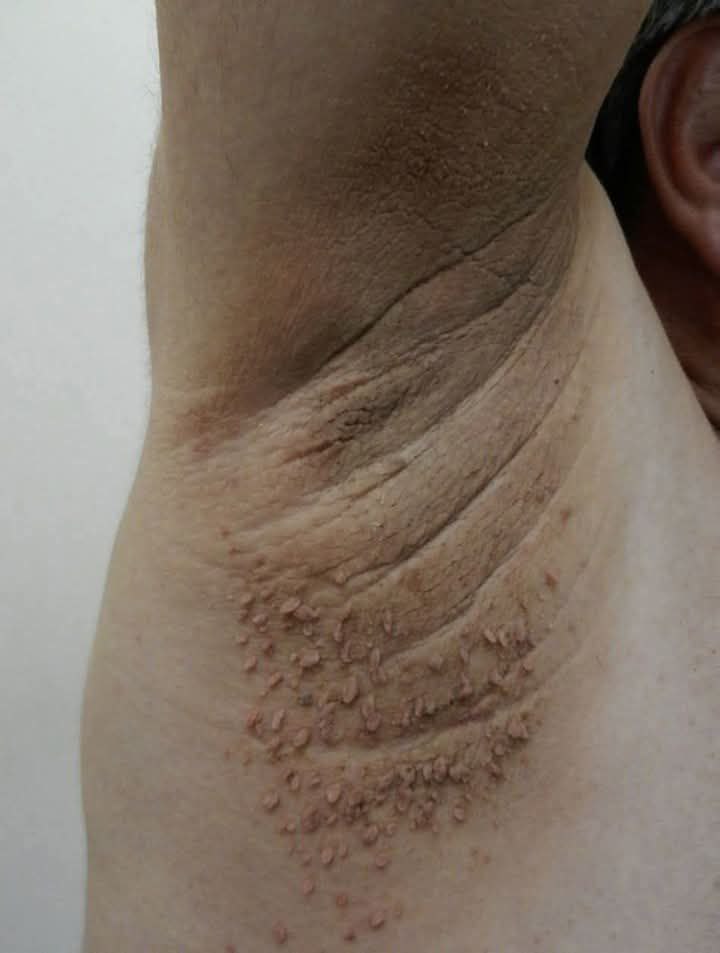
This condition is known as Acanthosis Nigricans, and it is commonly associated with insulin resistance and elevated blood sugar levels. Recognizing this early symptom could be key in preventing more serious health conditions such as type 2 diabetes.
What Is Acanthosis Nigricans?

Acanthosis Nigricans is a skin condition characterized by darkened, thickened, and velvety areas of skin, most commonly found in body folds such as:
- The back of the neck
- Armpits
- Groin area
The affected areas may feel soft or textured, and in some cases, may have increased hair growth. While the patches may resemble dirt, they cannot be washed or scrubbed off and should not be confused with poor hygiene.
What Causes Acanthosis Nigricans?
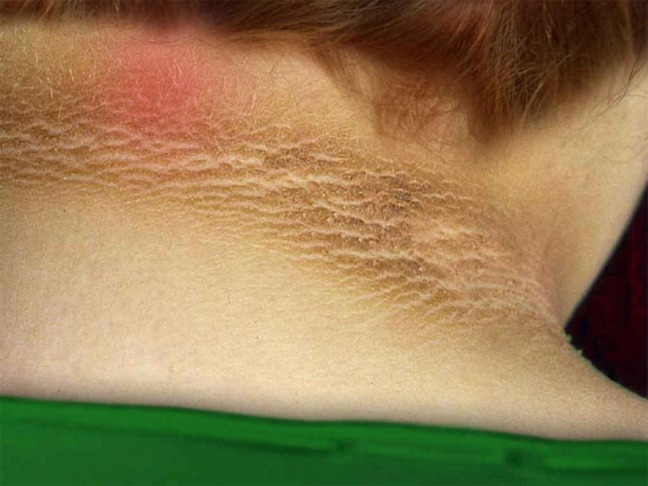
This condition is not a disease itself, but rather a visible sign of an underlying medical issue. Common causes include:
- Insulin resistance, often seen in individuals with prediabetes or type 2 diabetes
- Obesity, especially in children and adolescents
- Hormonal disorders
- Genetic factors
- In rare cases, medications or tumors
According to healthcare professionals, children and adults with obesity who develop Acanthosis Nigricans may be at increased risk of developing type 2 diabetes, making it a useful early warning sign.
A Doctor’s Insight: A Public Health Reminder
Dr. Hafizah Mohamed, a medical professional and member of the #medtweetMY health awareness community, recently shared on social media that darkened skin patches on the neck — particularly in children — could be an early sign of rising blood sugar levels.
“This isn’t just a buildup of dead skin cells. If your child or someone you know has these patches, it may be time to check their blood sugar,” she advised.
Dr. Hafizah emphasized that these patches are not itchy and generally don’t cause discomfort. If the area is itchy, red, or painful, it may be a different skin condition such as eczema, which would require different treatment.
How to Check Blood Sugar Levels
Many pharmacies offer on-site blood glucose testing, and blood glucose meters are available for home use. If you’re concerned about dark patches of skin or other symptoms, it’s best to speak with a general practitioner who can provide a diagnosis and further testing.
Checking blood sugar regularly can help identify early signs of prediabetes and allow for lifestyle changes or medical intervention before more serious complications develop.
Other Possible Conditions: Not Always Diabetes
It’s important to note that not all dark patches are caused by Acanthosis Nigricans. Another condition that can look similar is Terra Firma-Forme Dermatosis (TFFD). This harmless skin condition presents as brown or black plaques and can often be removed with 70% isopropyl alcohol swabbing.
If you notice dark spots on the skin that resemble dirt but don’t wash off easily, a healthcare provider can help determine whether it’s TFFD, Acanthosis Nigricans, or another dermatological condition.
When to See a Doctor
You should consult a healthcare provider if:
- You or your child develops dark, thick patches of skin suddenly
- The area spreads or becomes irritated
- There is a family history of diabetes or metabolic conditions
- You experience other symptoms like increased thirst, frequent urination, or fatigue
Early medical consultation can lead to early intervention, improving long-term health outcomes.
Prevention and Lifestyle Tips
If Acanthosis Nigricans is related to insulin resistance or obesity, the following steps may help manage or reduce its appearance:
- Maintain a balanced, healthy diet rich in vegetables, whole grains, and lean protein
- Increase physical activity, aiming for at least 30 minutes most days of the week
- Manage body weight through sustainable lifestyle changes
- Avoid sugary drinks and processed foods
- Have regular health screenings for blood sugar and cholesterol
In some cases, doctors may prescribe topical treatments or medications to manage the appearance of the skin, but addressing the underlying cause is the most important step.
Conclusion: Stay Informed, Stay Proactive
Dark patches on the skin — especially on the neck or underarms — may seem harmless, but they could be early indicators of blood sugar imbalance or metabolic changes. While not always a cause for alarm, these symptoms deserve attention.
Consulting a healthcare provider for evaluation can help rule out serious concerns and provide peace of mind. As always, maintaining a healthy lifestyle and being aware of physical changes are important parts of overall wellness.
On my birthday, my sister smashed the cake straight into my face, laughing as she watched me fall backward, blood mixing with the frosting. Everyone said, “It’s just a joke.” But the next mo

On my birthday, my sister smashed the cake straight into my face, laughing as she watched me fall backward, blood mixing with the frosting. Everyone said, “It’s just a joke.”
But the next morning in the emergency room, the doctor studied my X-ray and immediately called 911—because what he saw… exposed a horrifying truth.
Part One: “It’s Just a Joke”
On my birthday, the room smelled like sugar and candles and cheap champagne. A pink cake sat in the center of the table, my name written across it in looping frosting. Everyone was laughing. Phones were out. Someone shouted for me to make a wish.
My sister stood closest to me.
She grinned, eyes bright with something that wasn’t kindness. Before I could even lean forward, her hands slammed the cake straight into my face.
The impact was harder than anyone expected.
I felt myself stumble backward, my heel catching on the rug. There was a sharp crack as my head hit the edge of the table, then the floor. For a split second, the room spun in white and pink. I tasted sugar—and then iron.
Blood mixed with frosting, dripping down my chin.
People screamed, then laughed nervously.
“Oh my God,” someone said, still chuckling. “It’s just a joke!”
My sister laughed the loudest. “Relax! You’re so dramatic.”
I tried to sit up. Pain exploded behind my eyes. My vision blurred, and the ceiling swayed like it was floating. Someone wiped my face with a napkin, smearing blood across my cheek.
“You’re fine,” my mother said quickly. “Don’t ruin the mood.”
I remember thinking how strange it was that my ears were ringing louder than the music.
I remember the taste of frosting as I swallowed blood.
I remember waking up hours later in my bed, alone, my head throbbing, my phone full of messages telling me not to be “too sensitive.”
By morning, I couldn’t lift my arm.

Part Two: The X-Ray That Changed Everything
The emergency room smelled like disinfectant and sleepless nights. The doctor asked how it happened. I hesitated, then said quietly, “I fell.”
He nodded, unconvinced, and ordered X-rays “just to be safe.”
I lay on the cold table staring at the ceiling, replaying the laughter over and over in my head. It’s just a joke. That sentence hurt almost as much as my skull.
When the doctor returned, he wasn’t smiling.
He stared at the image on the screen for a long time. Too long.
Then he left the room without a word.
Minutes later, he came back—with a nurse, a security officer, and his phone pressed to his ear.
“Yes,” he said quietly. “I need emergency services. Immediately.”
My heart started pounding. “What’s wrong?” I asked.
He turned to me, his voice careful. “This isn’t a simple fall.”
He pointed to the X-ray. Even I could see it—fine fractures branching like cracks in glass, not just in my skull, but along my collarbone and ribs. Old fractures. Healed wrong. Layered.
“These injuries happened at different times,” he said gently. “Some weeks apart. Some months.”
I stared at the screen, my mouth dry.
“I don’t understand,” I whispered.
He met my eyes. “This pattern isn’t accidental. And the impact that brought you in today could have killed you.”
The word killed echoed in my ears.
“Who did this to you?” he asked softly.
I thought of my sister’s grin. My parents’ laughter. All the times I’d been shoved, tripped, “joked” into walls. All the times I’d been told I was clumsy. Sensitive. Overreacting.
My hands began to shake.
“I think…” My voice broke. “I think it was never a joke.”
Part Three: When Laughter Turns Into Sirens
The police arrived quietly. Calmly. Like this wasn’t the first time they’d seen something like me.
They didn’t accuse. They asked questions.
Who was there last night?
Who pushed you?
How often do you get hurt?
For the first time, I didn’t minimize. I didn’t protect anyone. I told the truth.
By evening, my phone was exploding.
My mother crying.
My father furious.
My sister screaming that I had “ruined everything.”
“You’re exaggerating!” she yelled over voicemail. “It was cake! Everyone saw it!”
Everyone had seen it.
That was the horrifying truth.
Everyone had seen it—and laughed.
The investigation didn’t take long. Videos surfaced. Old medical records were reviewed. Witnesses contradicted themselves. Patterns became impossible to ignore.
What started as a “birthday prank” became an assault case.
What they called humor was documented as violence.
I was moved to a different room that night, monitored closely, safe for the first time in years. As I lay there, ice wrapped around my head, I realized something terrifying and freeing all at once:
If that cake hadn’t been smashed into my face…
If I hadn’t fallen just right…
The truth might have stayed buried forever.
Sometimes it takes breaking something visible to expose what’s been shattered for years.







